Moreover, MoCA scores correlated with oxygen saturation levels. Even though the mild OSA group performed similarly to the primary snoring group on total MoCA scores, impairment in the visuospatial/executive function and delayed recall domains was more prominent. Domains that were significantly impaired in the severe OSA group, compared to the primary snoring group, were delayed recall, visuospatial/executive function, and attention/concentration. Furthermore, defining MCI with a cutoff of 25/26, the moderate-to-severe OSA groups were more classified as MCI than the other groups.
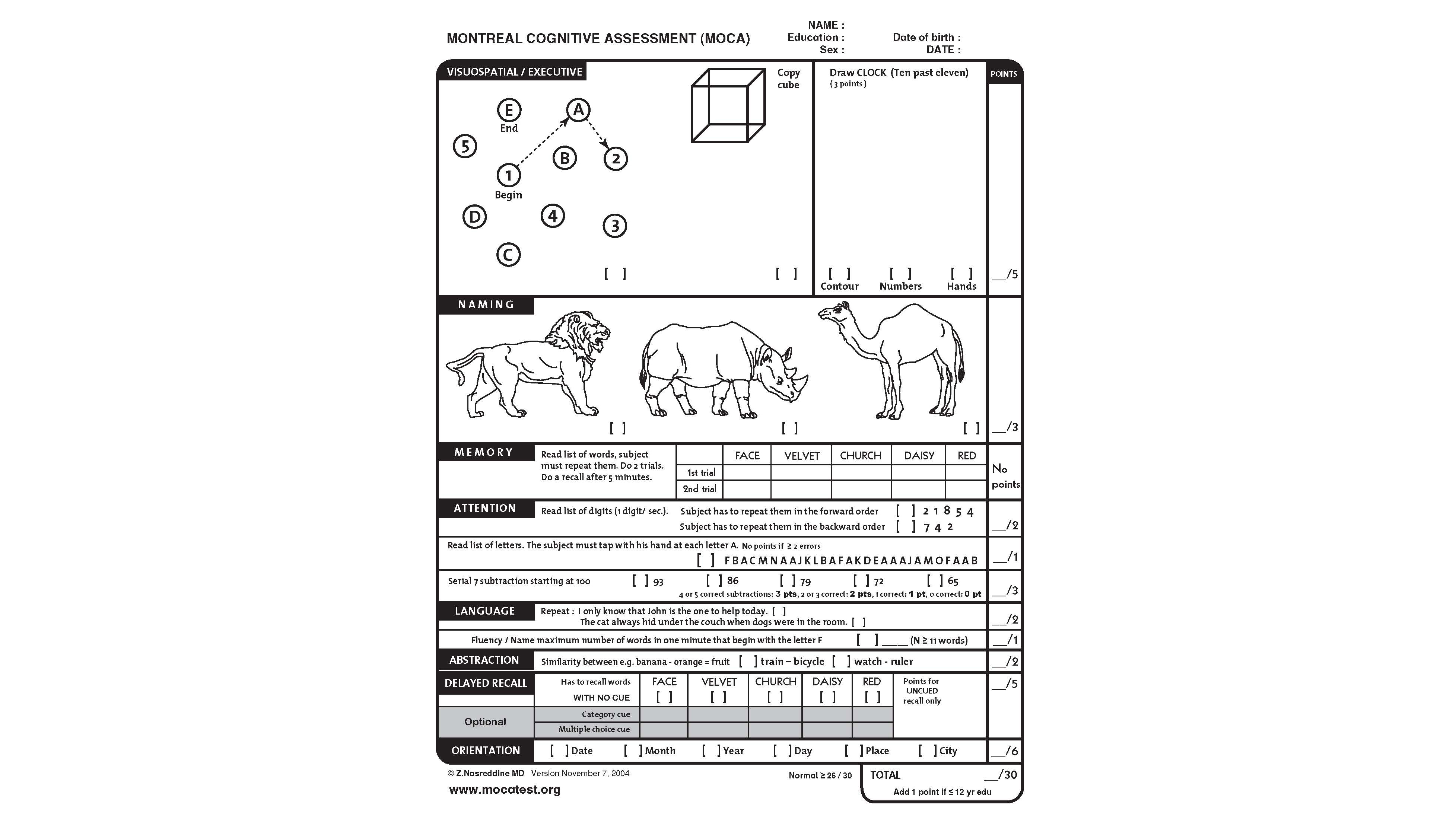

The scores of moderate-to-severe OSA groups were significantly lower than the scores of the primary snoring and mild OSA groups. The total MoCA scores progressively decreased as the severity of OSA increased. The groups were composed of primary snoring (AHI 40 events/h). , the MoCA was administered to 394 obstructive sleep apnea (OSA) patients categorized into four groups according to OSA severity based on the total number of apnea and hypopnea per hour of sleep (AHI), measured by polysomnography. Lower MoCA scores may represent other unmeasured confounders such as the extent of disease, location of tumor or previous treatment. Although, the MoCA scores correlated with the median OS, it is essential to clarify that cognitive impairment does not directly result in decreased survival. MoCA scores were superior to the MMSE scores as a prognostic marker.

After dichotomizing MoCA scores into two groups based on average scores (≥22 and 26, 22–26, and <22, were 61.7, 30.9 and 6.3 weeks, respectively. The survival prognostic value of the MoCA was studied among patients with brain metastases. 7.4 to predict conversion from MCI to AD with the MoCA total score and the MIS.Ĭognitive function is one of the survival prognostic factors and correlates with tumor volume in metastatic brain cancer. The mean time for AD conversion (n =114) was 17.5 months. This yields an annualized conversion rate of 60.3 % for the high-risk group and 35.2 % for the low-risk group. Using a cutoff of <20/30 for MoCA total score and <7/15 for MIS, the AD conversion rate was 90.5 % for participants with MCI who were below the cutoff on both measures and was 52.8 % for those who were above the cutoff on both measures. Within the average follow-up period of 18 months, 114 patients progressed to AD and 51 did not. Individual patients meeting the Petersen’s MCI criteria (n =165) were recruited from our memory clinic and tested with the MoCA at MCI diagnosis. We newly devised the memory index score (MIS) which was calculated by adding the number of words remembered in free delayed recall, category-cued recall, and multiple choice-cued recall multiplied by 3,2 and 1, respectively, with a score ranging from 0 to 15. In addition to the cognitive screening utility, the MoCA also provides the ability to predict AD conversion among patients with MCI. In general, studies recruiting a higher proportion of low educated subjects recommend lower cutoff scores for the education correction. There are many cutoff scores reported according to the level of education of the studied population. The cube copy, semantic fluency (substitution of letter F fluency), abstraction, serial-7 subtraction and naming in the Korean version of the MoCA positively correlated with education. Trail making test and digit span of the Japanese version of the MoCA significantly correlate with years of schooling. Education has been consistently reported around the world affecting total MoCA scores. Subsequent studies locally in Montreal suggest that to better adjust the MoCA for lower educated subjects, 2 points should be added to the total MoCA score for subjects with 4–9 years of education, and 1 point for 10–12 years of education.

Originally, the validation study for the MoCA recruited highly educated normal subjects, suggesting a correction of one added point for education of 12 years or less.
